Find a Listening Ear
The NICU may be a distant memory, but the effects of premature birth are often life-long. This is a place for you to say thank you to people who have helped you on your journey, vent your frustrations, or simply share your story. We’re here, and we’re listening.
Born in the 1950s
Thankyou for the opportunity to add my preemie experience. Just as you commented,, little is known about the experiences of adult preemies.
I was born in the mid 1950s in a small town in northern Montana, 30 miles from the Canadian border.
I developed a moderate case of ROP, & started wearing glasses at age 2. My mother noticed vision issues when I was 7 months old & said that when she placed food on my tray, I would move my face to about an inch away before I would take any. Although doctors were familiar with Retinopathy of Prematurity, there were no treatments for it, so mine progressed naturally. The macula’s should be positioned directly behind the pupil, but mine have shifted towards the center so that each one is near my nose, almost at the edges of the photo. The term for this is called ‘dragging’. I have always experienced sight challenges & was unable, for example to see the blackboard. My reading distance is about 4″ from my eyes.
In addition , I have some heavy duty sensory issues, neuropathy from Diabetes, as well as multiple neurological symptoms, learning disabilities, poor motor skills & brain processing issues as well as many other issues. Therapy for Sensory Dysfunction did not exist, nor did special education or alternative PE. I attended school with the ‘regular’ students. Teachers & educators were not aware of these issues, and rather than receiving the support that I needed, I was blamed, accused of being lazy & stupid, scolded for poor grades, when I was actually trying as hard as I could. There were no tutors for me either. PE was a nightmare every day, as I was unable to do sports, catch balls, swim, run, roller skate, or other activities. I spent an entire summer practicing to ride a bike when I was 12, because I had failed on earlier attempts. Having invisible disabilities in a time when no one was familiar with them (not even family or parents) was humiliating & embarrassing, & I spent my life ashamed of & hiding how I functioned. I knew that I was different than other people, but didnt know why. At home, I was scolded & blamed for not listening, following instructions, & getting poor grades.
I first asked a doctor when I was 16, why I was different & he just ignored my question, as did all other doctors & social workers. When I was 45, after a google search, I learned about Sensory Dysfunction & I tried to receive a diagnosis, only to learn that only children are treated for it. The private therapy is too costly for my budget, so I still have all the symptoms, even at my age. Sensory Dysfunction & many disorders from prematurity are not recognized as an ‘official’ condition & does not have a diagnostic medical code. In addition, most doctors feel that children ‘catch up’ with other children & eventually outgrow sensory issues.
2 years ago, I had a mild stroke & had brain scans done. This was the first time I looked at an image of my brain. I’m sure people’s brains vary, but mine didnt look right. Since then, I’ve read the articles that show brain scans of people with SPD & Autism in connection with a study from the University of San Francisco that shows variations in brains of people with sensory disorders.
I don’t say much about the issues I have to deal with on a daily basis, because people just don’t understand. They expect me to speak & respond as quickly as they do, don’t understand when I become confused or are unable to remember details to fill out medical forms, or follow a string of instructions.
I have ‘gotten by’ from writing everything down, such as new job instructions, to directions around office buildings, to instructions from doctors, as well as how to find my way to and from stores in malls and how to get to and from the bathroom and around hospital corridors.
For employment, I worked in retail, as office work was too hard on my eyes, then I went into the sewing machine industry, teaching classes on how to use sewing machines & sergers, as well as specialty classes. It probably sounds odd, that I can sew with my poor vision, but my close vision is better, so I really did ok. My ROP prevented me from driving, so I took public transportation to get to work locations, appointments etc.
Over the years, I have lived in 5 different states, have traveled to many different places using trains, busses, planes, alone & with spouses and friends. I love to cook & have done so since I was a teenager.
I was married at a young age & suspect that my invisible disabilities contributed to my ex wanting out. Maybe, he felt that I was too ‘needy’. Fortunately, later in life I met & married the sweetest, most understanding person & he is supportive & helpful in many different ways.
In concluding, I just wanted to say that as a formerly premature baby with no support or therapy, other than the eyeglasses, I feel that these experiences have made me a stronger more compassionate person & hope that all preemies can accomplish what they want & fulfill their dreams.
On May 31, 2012, I

On May 31, 2012, I was 6-months pregnant with my second child. On that day, I went to my doctor’s office for what was to be a routine checkup. However, that appointment turned out to be anything but “routine.” At that appointment, my doctor couldn’t locate my son’s heartbeat. I was immediately placed in an ambulance and with sirens blaring, I was transported to the nearest hospital. I was immediately prepped for an emergency C-section. I remember pleading with the OR nurse, terrified, “Please don’t take him out. It’s not time. He’s not ready,” even as part of me understood that this was my son’s only chance for survival.
My youngest son, Joshua, came into this world at 26-weeks gestation weighing just 2 lbs. at birth. It was the first time I heard the term, “Micro-preemie.”
Like most preemies, Joshua came into this world in critical condition and remained so for weeks to follow. On his second day of life, his brain hemorrhaged to a significant degree that when the doctor met with us, we had very little hope of Joshua recovering. All we knew in that moment was, Joshua might live. He may die. At best he could be severely disabled.
As my body had a negative reaction to the pain meds I was on, I didn’t get to meet Joshua until his 3rd day of life. Nothing in this world, no amount of preparation, explanations or advice could have ever prepared me for what I was about to witness. Instead of little blankies and stuffed animals surrounding him in a cute little bassinet like I had experienced with my first son…Joshua was in a what seemed to be to my untrained NICU eyes, a type of science project box which I later learned was called an isolette. There were monitors, wires and leads all stuck to his underdeveloped and fragile body while a ventilator worked to keep him alive. I wasn’t able to hold Joshua until almost 2-weeks after his birth. Holding him for the first time was bittersweet as I looked down and couldn’t see his little face through the ventilator mask and jaundice goggles, but once he was placed on my chest, as surreal as it felt, we were together again and I was determined to do everything I could for him. That meant pumping breastmilk for him every 3-4 hours, advocating for him and most importantly, keeping hope alive. It wouldn’t be until we were finally home that I was able to recall all the memories of those first few days in the NICU. The fog had finally lifted a bit enough for me to understand what we had truly gone through as a family and how much it affected us and would continue to affect us emotionally even years later.
Joshua spent 129 days in the NICU. During his 129 days, we watched our youngest son fight many battles. Joshua developed acidosis early on, respiratory distress, PDA, he sustained a bilateral grade III/IV IVH and had a gastrostomy tube surgery, among many other complications. 129 days. That number has been ingrained in my memory and has irrevocably changed who I am at my core. That’s 129 days of fear, tears and exhaustion. It’s 129 days of having to walk away and leave my child in the care of strangers. But it was also 129 days of hope, memories and life lessons as I witnessed my youngest child tenaciously fight for his right to be here.
Now, what does life look like for our family today? Well, there have been many changes in our household since Joshua’s early arrival. Once we got Joshua home and thriving, my husband was diagnosed with stage IV Renal Cell Carcinoma and at the tender age of 40, he passed away only 9-months post diagnosis. Suddenly I found myself thrown into the world of solo parenting two grief-stricken children and one of them, (Joshua) with special needs. As you know, prematurity doesn’t end in the NICU. It is a life-long journey with many bumps along the way.
Today, Joshua is a happy, rambunctious 7-year old who loves Disney Cars, Hot Wheels, singing and dancing. He is in a special education program at his school and continues to receive different forms of therapy. Joshua is autistic and has some speech delays and fine motor delays and every day brings new challenges, but he is also the top reader in his class and is incredibly intelligent with a laugh that melts even the hardest of hearts and Joshua’s journey continues to teach me grace, acceptance and bravery in our ever-changing world.
Born at roughly 26 weeks, now getting a masters degree.

I was born at roughly 26 gestational weeks with several issues at birth. I had undeveloped lungs, a heart murmur and a few days after my birth I was diagnosed with an IVH, which is short for Intraventricular Hemorrhage. I was diagnosed with the most severe case at the time a level 5 bleed , which is now downgraded to a level 4 bleed. I stayed in the NICU for another 6 months fighting for my life. Unfortunately, my doctors told my parents that there was a very high possibility that I would be mentally disabled due to the severity of the bleed and not placing a shunt inside my head to relieve some of the pressure and decrease swelling.
Over the next couple of years my parents participated in Early Intervention Services with me to really help give me develop my motor and cognitive skills aside from what the doctors told them. My mother and father would give me their own special exercises at home to further help me with my motor and cognitive skills as well. I did a lot of things way slower than other toddlers my age for example walking , talking and even being unable to hear for years. My mother would take small pots and pans and clings them together softly to try and test my hearing at home to hopefully get a response from me. I struggled doing so many things over the years.
I went from receiving assistance from the state every month in the first grade until I made straight A’s to the third grade, where I started to read at a ninth grade level and eventually tested into the Gifted Education Program in my school district that same year. My parents never allowed me to feel any different from anyone else as the years went by. I was able to watch my dad firsthand save complete strangers on their worst day ever from wrecked vehicles and burning homes and buildings as a firefighter for years . My mom would read to me every night as a child and as I became older she would make my younger siblings and I read several books in the summer and write a book report for each book that I had read that week. I played several sports growing up also.
I said all of that to say this: the power of giving can change someone’s life. I ask that each and everyone reading this message today gives their preemie a fighting chance…. Attitudes are more important than facts….
Today I am an electrical engineer. I just recently finished my masters at Georgia Institute of Technology in Biomedical Innovation & Development. I hope to someday develop devices that help give other preemies like myself and their families hope for a better tomorrow and a healthier future.
My son zayden was born
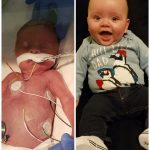
My son zayden was born 7 weeks early just 7 months ago. He is my first child so I honestly never even thought of this scenario. When he was born he needed breathing assistance, he was placed on a CPAP and it caused a tension pneumothorax and almost killed my son. He then had a chest tube placed and was intubated, a few days after being intubated we found out he had a ecoli infection. All of this was too much on our not even 2 week old son and that night he went into shock and respiratory failure. It was the scariest moment of our life, me and my husband didn’t know that to think. He received tons of medications and a blood transfusion and he got better slowly. He remained in the NICU for 6 weeks before he could come home with us. He is now a happy, healthy 7 month old. It is amazing how far these little babies can fight!
When I was 34 weeks
When I was 34 weeks preg, I went out for coffee with a friend and my water burst everywhere! Very movie like if you ask me! That marked the beginning of my baby boy’s entrance into the world becoming. The beginning of a very difficult emotional roller-coaster and for us becoming Mummy and Daddy.
That same night, my partner and I were told to come into the hospital. From then on they explained that I was not in labour but because my waters had broken, they needed to monitor the baby and me in hospital. I spent 10 days in hospital when originally they said 3. I had family and friends texting and calling every hour, which was beautiful, although it sometimes felt too overwhelming when my partner and I didn’t even know what way the day would go. I spent everyday being told that if baby’s heart rate didn’t do a certain pattern, then we would need to do an emergency C-section. Some days his heart beat wouldn’t meet their requirements and then later on it would. We were in a constant place of uncertainty for 10 days. That was until a tactless ultrasound lady told us that ‘its worse than last time’ – meaning my baby was sending blood to vital organs. Basically, he had gone into survival mode.
The next day, I was induced but my baby couldn’t cope with the contractions. He was small for his gestational age and had no amniotic fluid to protect him through each contraction. About an hour into labour, I had a cesarean. My baby boy was born on Valentine’s Day.
The next 3 weeks my partner and I spent in special care with our tiny little 1.7kg baby boy. He was never sick, just small and premature. The time spent in special care was the hardest part for me. I didn’t want to be in hospital, yet the nurses would say ‘you can stay here as long as you want! All night and day’ – making me feel guilty for wanting to go home. But each time I left, I cried my eyes out as my baby boy wasn’t with me. The urge I got as a mother was so intense, all I wanted was to have him on my chest, skin to skin, helping him grow. It was a fight I had with my self everyday, wanting to be with him, but wanting to be home. I felt guilty and sad and angry and lost. I wasn’t me anymore, I was someone else, making their way through an ocean of emotions, trying to heal from major stomach surgery and trying to help my little boy learn how to feed on the breast, and not through a nasal gastrictube. I had to see him have this put in, it is uncomfortable for a baby and it was the first time I’d seen him really cry. I held his little hand while this nurse who fumbled with it got it wrong and had to get another nurse to help her try again. This little man having a tube from his nose into his stomach. I cried and cried and cried. I saw it logically, “its okay, it doesn’t hurt him” but my god, I was not coping. My partner was so strong for these 3 weeks. So strong, every time I cried he would give me a speech of all the ways I was doing well.
From day one after surgery, I was handed about 2 pamphlets a day of information. I was bombarded by lactation consultants telling me information about how to breast feed and telling me ‘you should really get up in the night to express’ although I had explained to her that I had tried this and that it was really getting me down (my way of saying I wanted to jump off my balcony).
Expressing – my god, what a miserable thing to do. That’s how it felt at the time. That I was chained to this machine every 3 hours that pumped me like a cow. I never felt like I could relax, or that I was free. I felt a need to pump an amount this piece of paper told me to get to “by day 7 I should be pumping 700ml a day” I’d tell myself. That was my goal, I couldn’t do it straight away and my god, my anxiety through me into a shitty place. I was a prisoner of my anxiety. I cried everyday. I held my baby on my chest for 3-12 hours a day, usually 6. Two feeds, trying to teach him to feed, feeling like a queen when he latched on and fed for 5 mins, and feeling like I was never going home when my poor little bubba was too busy trying to stay warm and keep body fat to breast feed.
The nurses would tell me to ‘go to groups with other parents” and that I could “stay here as long as I want”, when all I wanted was someone to give me permission to go home, to be told I was doing enough. My partner told me this everyday. I had to be convinced every single day that I wasn’t doing something wrong by leaving my little man, by wanting to go. Wanting to go home, that felt like my biggest failure.
My Daughter
My daughter was born at 24 weeks 6 days. She was a tiny fragile thing amidst the cords and lights. A mere 555 grams (1lb 4oz) when born. We spent 132 days in the NICU. Truth be told, if I hadn’t chronicled most of it, I still get lost in details. So much has happened.
My first child. I expected to go full term, as most women do. My baby shower was in the planning stages. I had bought one little outfit for her.
Then when I was about 24+2 and had a nurse visit. From there, I was told to go straight to labor and delivery. Panicking, I drove there fast as I could. Turns out my blood pressure had skyrocketed, despite the blood pressure medication I was on all pregnancy. I checked in that Monday, had her that Friday and didn’t leave for 9 days. Preeclampsia and IUGR.
132 very long days went by before she was strong enough to come home. She was one of the lucky ones – no brain bleeds, mild retinopathy of prematurity, no major problems. She needed multiple blood transfusions, a chest tube for a collapsed lung, and a spinal tap. Smaller problems but nothing that couldn’t be controlled. A few touch and go moments in the beginning. Her nurses were amazing. I came to know them well.
Fast forward to that first year. She was on oxygen for a year. She was diagnosed in the NICU with Pulmonary Hypertension, which can be fatal to kids. Around age 3 they told me it had resolved. She had a little occupational therapy until age 3. All 5 specialists that she saw tapered off after 3 for her. Then she began her “normal” childhood, minus doctors and oxygen and medications.
She is 7 now. Tall and thin like her dad. The only complication we deal with that is directly associated with being a preemie is asthma. It’s mild, but she’s on meds for it.
She’s incredibly bright, and is even in gifted and talented at school for the past 3 years.
I couldn’t be more grateful to the nurses and staff who held her when I couldn’t, who treated my daughter as if she was their own. I’m not sure where we’d be if that was not the case.
Grateful and thankful,
Tomarra and Lily
Preemie Deb

I don’t just run Preemie Crystal Ball, I get it from all sides. Not only did I give birth to my daughter Becky in 2003 but I knew from my mother that I had been a “little early.” That was all I knew and my OB didn’t care one whit about that nugget of information and told me that it was my first pregnancy and I would be “late.” A month later I was staring at my newborn preemie daughter as she struggled against the medical equipment in her incubator in the NICU.
Fast forward a decade later after my parents had both passed away. My brother cleaned out the house and found a bunch of items for me. Among my silly childish letters to my parents lay a telegram. A person had sent a note saying that I had been born a month early but that I “was okay.” Wow . . . I knew then that I was officially a preemie and suddenly a lot of things made a huge amount of sense. From lung issues, to struggles with coordination to mental health challenges as a teen and also with my daughter’s early birth. It all clicked into place.
We need to do better with neonatology in terms of helping these tiny babies once born, truly thrive beyond birth and beyond the NICU. To do otherwise after all of the huge investment of medical assistance is an insult. And I am speaking about all preemies, not just the tiniest of tiny babies, the micro-preemie.
